Ongoing Knee Pain?
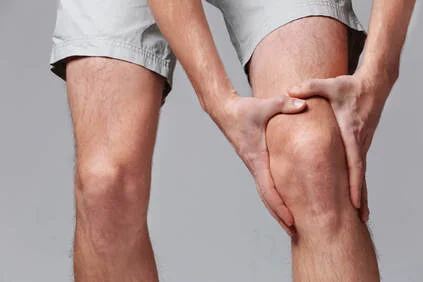
You’ve powered through 9km of your 10km run on a sunny Sunday morning. You start thinking about your Sunday morning coffee and your relaxing afternoon ahead when you start to feel this sharp pain at the front of your knee. You keep running thinking it will go away but it doesn’t, it only gets worse. You end up stopping and have to walk home. You put some ice on your knee and rest it and hope the pain dissipates however, weeks go on and that nagging knee pain is still there. This feeling is a terrible one experienced by many runners across the world, and is commonly called “runners knee”, or more formally patellofemoral pain syndrome (PFPS) and is one of the most common knee related conditions experienced by athletes. In fact, the annual prevalence of PFPS is reported to be 22.7% in the general population(1). Here is a little background information on PFPS and how to deal with it to get back on the running track this season.

PFPS is pain experienced in the front part of the knee, particularly on/around the kneecap. It occurs when there are muscular imbalances present; tight muscles in one area and weak muscles in another, that put abnormal stress upon the joint(2). Pain is typically aggravated with activities that load or require repetitive use of the knee, such as sports involving running and jumping, stairs, walking and squatting. Treatment is conservative and should address the functional cause of the symptoms.
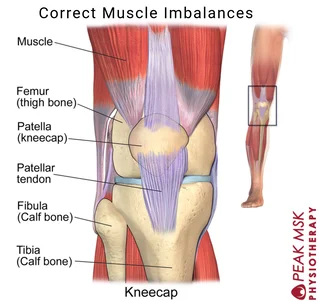
Risk factors that make an individual more susceptible to developing PFPS include; age, sex, certain sports and foot alignment(3). PFPS typically affects adolescents and young adults under the age of 50. Women are twice as likely as men to develop PFPS due to the wider pelvic hip alignment in females. Participating in sports that involve running and jumping can increase the likelihood of developing PFPS as these sports place a high level of stress on the knee joint. Additionally, having flat feet also places additional stress on the knee joint which increases the likelihood of developing PFPS.
2. Fagan V, Delahunt E. Patellofemoral pain syndrome: a review on the associated neuromuscular deficits and current treatment options. British Journal of Sports Medicine. 2008;42:789-795.
3. Waryasz, G., & McDermott, A. Patellofemoral pain syndrome (PFPS): a systematic review of anatomy and potential risk factors. Dynamic Medicine 2008;7(1):1476-5918-7-9.
4. Nascimento LR, Teixeira-Salmela LF, Souza RB & Resende RA. Hip and Knee Strengthening Is More Effective Than Knee Strengthening Alone for Reducing Pain and Improving Activity in Individuals With Patellofemoral Pain: A Systematic Review With Meta-analysis. J Orthop Sports Phys Ther. 2018;(1):19-31.