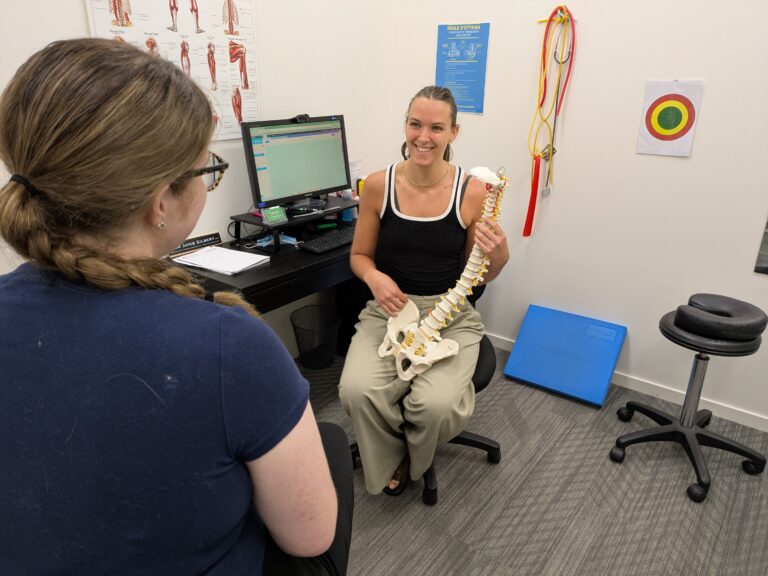
Osteoarthritis is the type of arthritis that happens over time as the cartilage layers change over time making them less resilient. Cartilage is the spongy tissue that coats the ends of bones in joints and acts as a shock absorber. Normally, damaged cartilage is constantly being repaired as old cartilage is degraded. When the balance between degradation and repair is thrown off, cartilage thinning occurs. As a result of cartilage thinning, the joint has more friction causing a joint to become inflamed.
What’s the Difference Between Osteoarthritis and Rheumatoid Arthritis?
What are the Risk Factors For Osteoarthritis?
While there is still much to learn on the subject, some known risks factors include:
- Overweight: increases load through the knee
- Age and gender the older you are
- Gender: women over 50 are more likely to have OA than men over 50
- Genetics
- Trauma: previous injury to the knee, including sports injuries, can lead to OA Knee.
- Repetitive stress injuries: which are usually associated with certain occupations, particularly those that involve kneeling or squatting.
What Are the Most Common Symptoms of Osteoarthritis?
Pain is the most common symptom of osteoarthritis, occurring primarily when the joint is moved, rarely at rest. Other symptoms include:
- Limited range of motion
- Crackling sounds
- Stiffness
- Buckling or locking of the joint
- Swelling / inflamed joints
How is Knee OA Diagnosed?
What Are My Treatment Options?
It depends on the severity. Initial treatment is generally directed at non-invasive pain management. Pain related to joint osteoarthritis may have different causes, depending on the individual and the stage of the disease.
We ensure individualised treatment prescription based on your examination findings. This is best current practice (1).
In general, treatment is
Specific targeted exercise to address, strength, agility, coordination to cushion joints, stimulate healthy cartilage and minimise friction.
Also included is:
- Health and behaviour modifications, such as patient education, physiotherapy, exercise, weight loss, and bracing.
- Physiotherapy is aimed towards strengthening muscles around the joint and participating in a low impact graded cardiovascular exercise program.
- Treatment options also include medication for pain relief such as anti-inflammatories or Panadol.
- Corticosteroid injections are also an option.
- Platelet Rich Plasma injections are becoming more common place with good outcomes in the short term. The longer-term benefits are still being investigated by researchers.
What If Non-Surgical Treatment Doesn’t Work for Me?
When quality of life and makes daily activities difficult to perform then a joint replacement maybe recommended whereby the knee joint is replaced with an artificial prosthesis. This surgical procedure has been shown to reduce pain, enhance quality of life, and improve your ability to perform everyday activities with fewer or no restrictions.
References
- Curr Opin Rheumatol. 2018 Mar;30(2):151-159