Despite the concept of piriformis syndrome being proposed over 80 years ago, the theory is still controversial, with some research questioning its existence entirely. One of the issues surrounding piriformis syndrome is the symptoms are similar to neurological pain referring from the back as well as many other conditions. Symptoms of piriformis syndrome are said to include numbness, or the feeling of pins and needles, pain around the hip and buttocks, an inability to sit for a prolonged period and pain in the buttocks that gets worse with hip movement.
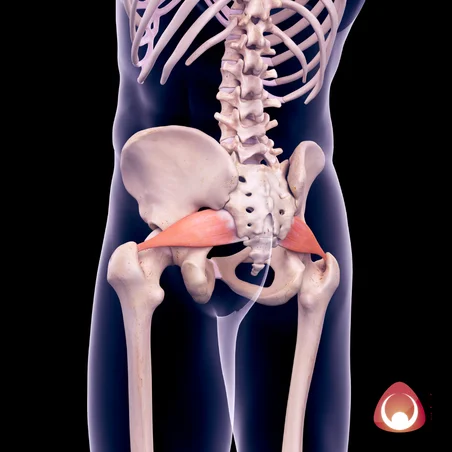
The theory behind the syndrome is that a taut or abnormally shaped piriformis muscle can compress the sciatic nerve (which passes by the piriformis) and cause sciatic pain. While there are currently no universally accepted tests to diagnose piriformis syndrome, some practitioners argue that stretching, activating or palpating the deep gluteal region and the piriformis can rule in or out piriformis syndrome. Of note however is a recent study found that ultrasound could potentially be a method of diagnosis for piriformis syndrome. This research showed that patients thought to have piriformis syndrome had an enlarged piriformis and sciatic nerve on their injured side, when compared to their asymptomatic side and to healthy volunteers. More research is needed into the topic however. On the basis that there are no reliable ways to diagnose piriformis syndrome, if a diagnosis is made, it is generally done so when all other sources of sciatic pain are excluded.
Despite the exact pathophysiology of the syndrome being debated, the direction for treatment is relatively straight forward and is treated like most other muscular dysfunction syndromes. Myofascial release, stretching, massage, ergonomic modification, and trigger point release are some of the recommended treatment options for Piriformis syndrome.
Despite the exact pathophysiology of the syndrome being debated, the direction for treatment is relatively straight forward and is treated like most other muscular dysfunction syndromes. Myofascial release, stretching, massage, ergonomic modification, and trigger point release are some of the recommended treatment options for Piriformis syndrome.
Takeaway:
Given the anatomy, it is reasonable to believe that piriformis has the possibility of irritating the sciatic nerve and causing sciatic neuralgia. At this stage however, there is no clear-cut diagnostic procedure to diagnose piriformis syndrome. The exception to this is a recent study that found ultrasound could potentially be a method of diagnosis for piriformis syndrome, however further supporting research is required. The diagnosis of piriformis syndrome could be made once all other probable sources of sciatic neuralgia are ruled out. Should this be the case then it would be reasonable to assume the presentation would respond to myofascial release, stretching, massage, ergonomic modification, and trigger point release.
Watch our video on Piriformis Syndrome for more information. Click the button below!